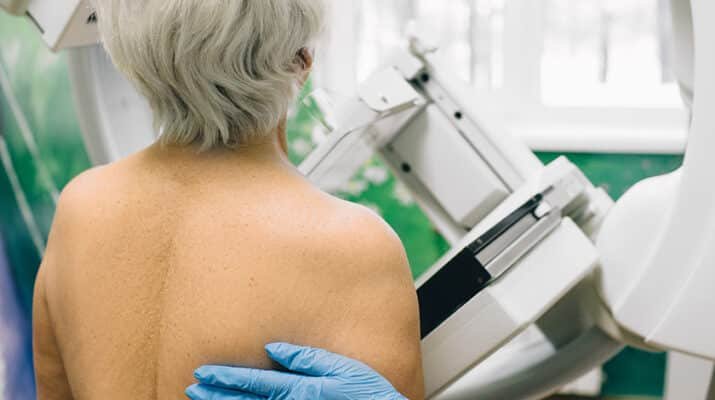
Study: Some women over 70, if diagnosed with breast cancer, need to weigh if pursuing treatment is the right course
By Deborah Jeanne Sergeant
A recent study of 54,635 women ages 70-plus by Yale School of Medicine indicates that 31% of women ages 70-74 and 47% of those 75-84 were possibly “over-diagnosed” with breast cancer.
The term means that they were found to have a kind of breast cancer that is slow growing and that treatment would likely not extend their lives or improve their quality of life.
In fact, pursuing treatment such as lumpectomy, mastectomy or chemotherapy would dramatically decrease quality of life.
“There is no exact age at which women should stop getting mammograms,” said Susan Brown, registered nurse, senior director of Health Information and Publications at Susan G. Komen headquartered in Dallas. “Breast cancer risk increases with age, and mammography doesn’t appear to be less effective in women 70 and older. However, there are risks of mammography in older women, including over-diagnosis and over-treatment, when a cancer that would not have caused problems if untreated is treated and the person is subjected to side effects without receiving any real benefit from the treatment.
“Many major health organizations recommend women ages 70 and older continue to get regular mammograms as long as they are in good health and could benefit from treatment if breast cancer were found.”
She added that poor health may cause some women may stop routine breast cancer screening, as would the presence of other health issues that would take precedent. The organization’s stance is that women should be able to access regular screening mammograms as long as they and their providers think they should.
When to stop mammography—and when to start—relies upon many health factors.
Robert Smith, physician, vice president of Early Cancer Detection Science for the American Cancer Society, said that women at high risk may start with annual mammograms earlier than other women, typically around age 30.
“Some women with a first-degree relative like a mother or a sister who was diagnosed at a young age have been advised to begin screening ten years before the age that relative was when she was diagnosed,” Smith said. “Women who receive regular mammograms are more likely to have breast cancer diagnosed earlier, less likely to need aggressive treatments, and more likely to be cured. However, mammograms are not infallible; they may miss some cancers, and even when issues are found in an initial screen, further testing may be needed to confirm the presence of cancer.”
Those who are 55 and older may choose to switch to every other year. But Smith said those who are 75 or older can continue annual screening as long as they remain in good health and expect to live at least another 10 years.
Onondaga County Health Department Medical director James Alexander, physician, said that most organizations currently state that through age 75 is reasonable as for how long to receive mammography.
“After that, it comes down to ‘shared decision making,’” he said. “You sit down with the patient and talk about their desire to continue breast screening and what would they do if they had a positive. Do all the women and their family live to be 100 with healthy, active, productive lives? That 75-year-old is different from one who doesn’t have those great genetics of longevity. You have to really consider also the general health status of the patient and incorporate that into your shared decision making.”
He said that a woman who is 75 and not well, who has advanced heart disease is not as likely to continue to seek mammography.
“As you get older, they’re going to find more breast cancers present, but maybe they wouldn’t be aggressive or advance quickly,” he said. “It maybe won’t be life threatening. What we need to figure out is what is the appropriate intervention in that case and how much screening do we continue?”
The treatment of a tumor at this stage in life might be progesterone for a slow-growing tumor rather than aggressive treatment with surgery or chemotherapy, which would decrease the quality of the life the woman likely has left. Alexander calls this a “risk-based analysis” to decide about the appropriate care on an individual basis rather than stating that a certain age is a hard-and-fast cutoff.