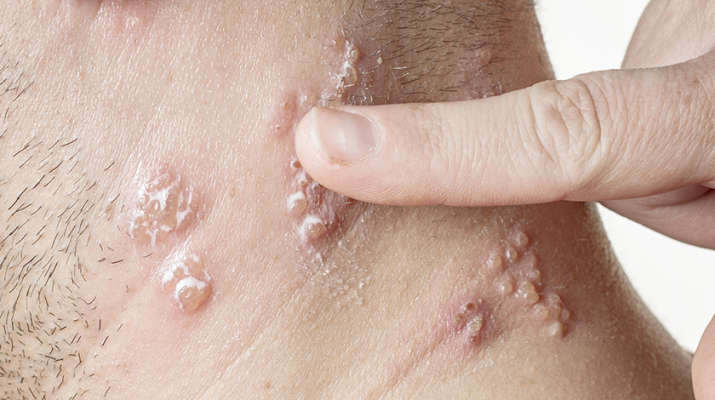
For experts, it’s a no brainer. If you had chickenpox as a child and are over 50, you should get the vaccine
By Deborah Jeanne Sergeant
You faithfully receive your flu vaccination every fall, but have you thought about shingles?
If you’re like most people who had chickenpox as a child, you have a risk of developing shingles once you hit your 50s or 60s.
That’s why physicians — such as Ramsay Farah of Syracuse — recommend that adults age 50 and older who have had chickenpox should receive shingles vaccine.
Farah is an associate professor of medicine, pathology and ear nose and throat at Upstate Medical University. He also works as a dermatologist at his family’s practice, Farah Dermatology in Syracuse.
Caused by the varicella-zoster virus, shingles occurs when the virus that causes chickenpox reactivates later in life, usually after age 50.
“If the zoster spreads beyond a small area, it can result in hepatitis, pneumonitis, or encephalitis,” Farah said. “This happens very rarely, but is more of a risk in severely debilitated or immunocompromised patients.
“If the shingles occurs on the head and neck area, and involves important structures such as the eye one can also get conjunctivitis, scleritis, episcleritis, keratitis iridocyclitis, Argyll-Robertson pupil, glaucoma, retinitis, choroiditis, optic neuritis, optic atrophy, retrobulbar neuritis, exophthalmos, lid retraction, ptosis, and extraocular muscle palsies.”
Farah added that the only contraindications to the shingles vaccine include allergies to one or more of the components of the vaccine, gelatin or neomycin. The other contraindications are conditions or medication that suppress the immune system, such as chemotherapy drugs.
Local reaction at the injection site is the most common side effect. Some insurance plans cover shingles vaccination.
Shingles start out with a sensation of burning, pain or tingling in an area of the body, sometimes as a band, but only on one side of the body. Within two days, infectious lesions form (once they form a crust, the patient isn’t contagious).
People at higher risk for shingles include those who have experienced chickenpox and who currently have a depressed immune system because of stress, injury, medication or unrelated disease.
“One in three people will get shingles during their lifetime, and at least half of all people 85 and older have had the ailment,” Farah said.
He added that since 1993, the incidence of shingles has nearly doubled in the adult US population. It’s unclear as to why shingles is on the rise, but “the benefits outweigh the risks for most individuals to actually get the vaccine.”
Elizabeth Arthur, dermatologist at Helendale Dermatology & Medical Spa in Rochester, agrees. She had shingles last summer at age 53. The illness landed her in the hospital five days. She advises patients to seek treatment for the disease within the first two days, since this tends to lessen its effects and reduce the risk of post-herpetic neuralgia, lifelong flare-ups in the same place manifesting lesions. About 20 percent of patients experience post-herpetic neuralgia.
“The pain afterwards can be debilitating,” Arthur said. “For me, it was the worst pain I’ve ever had in my life.”
Some describe it as burning, stinging, shooting pain in the skin that any slight contact sets off, such as clothing brushing against the skin.
Topical preparations can reduce pain at the site, while oral anti-viral medication can help reduce the duration and risk of post-herpetic pain.
The vaccine reduces patients’ risk of developing shingles by 50 percent.
“I wondered if it made a big difference,” Arthur said. “After having it, I’d say, absolutely. Even a mild case, if you can reduce it, isn’t that better?”
Vaccination can also help prevent the spread of illness to others who are not or cannot be vaccinated, such as yet-unvaccinated babies, who can develop chickenpox from an adult’s case of shingles.
Anyone approaching 50 should discuss shingles vaccination with a primary care provider.